Preparing for an Emergency
In northern Israel, Galilee Medical Center is already moving patients, canceling procedures, and training doctors in anticipation of a second front opening
Roni Albert
Roni Albert

Roni Albert

Roni Albert
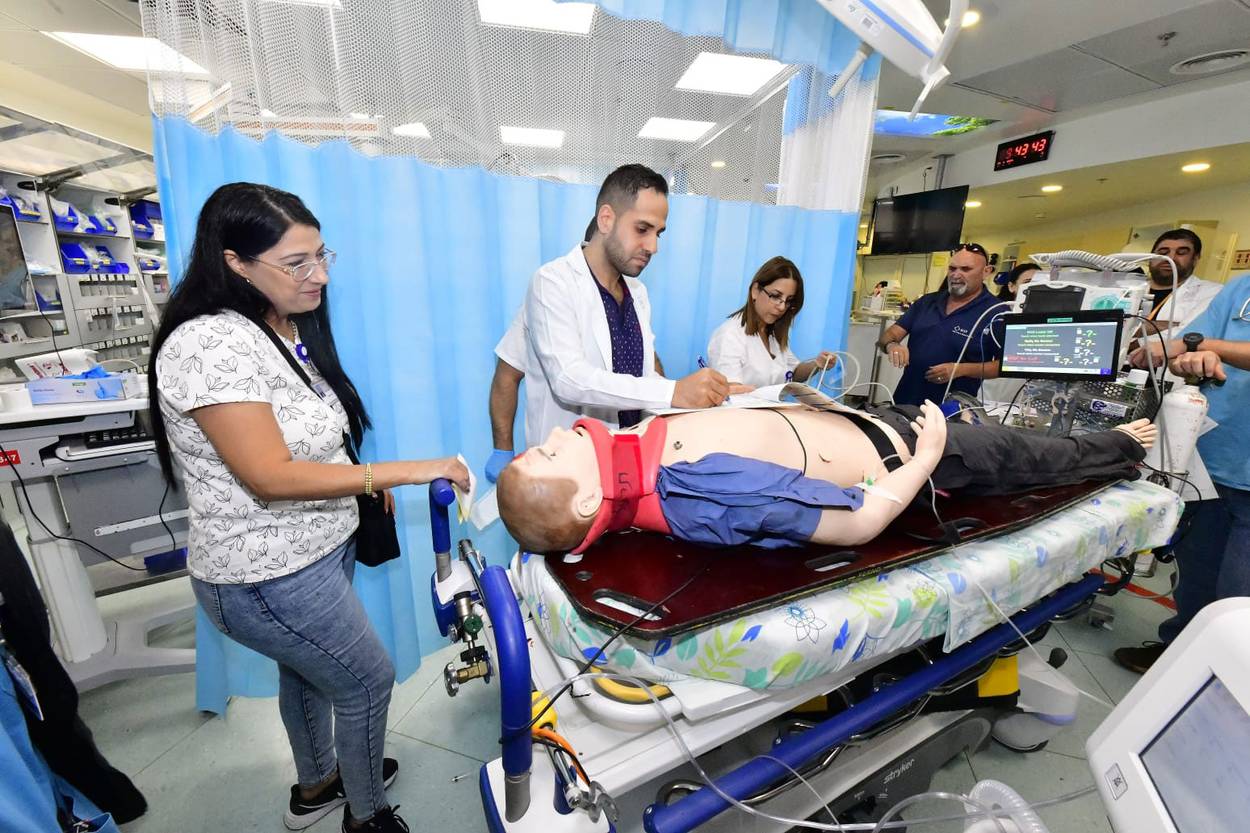
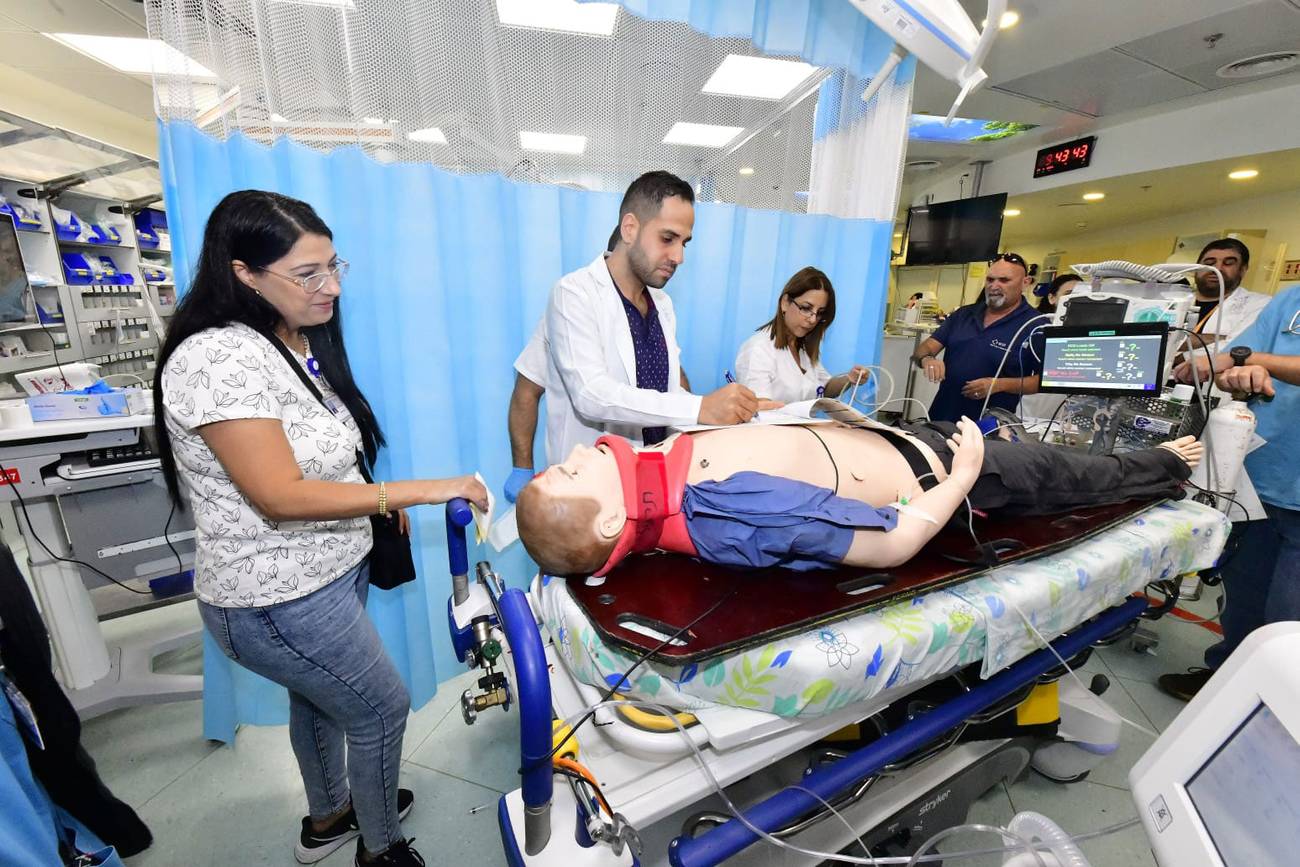
On the morning of Wednesday, Oct. 25, a patient at Israel’s Galilee Medical Center emitted deep, painful sighs as a medical professional administered treatment.
The “patient” was a mannequin, and the dozen doctors, nurses, and administrators gathered around its bed were learning from the scenarios presented there and at two adjacent beds: patients with an airway obstruction, difficulty breathing, and a circulation problem. The presenters were emergency-department doctors and nurses running the simulations to train colleagues in other departments.
The drill was held to prepare for an emergency.
Here in the coastal town of Nahariya in northern Israel, that emergency would be a second war front opening, as residents and analysts expect, given the Lebanese terrorist organization Hezbollah launching raids and missiles at Israeli military and civilian targets with greater frequency while piggybacking on Hamas’ Oct. 7 massacre of Israelis 110 miles to the south.
Should Hezbollah’s attacks escalate to war, large numbers of Israeli soldiers and civilians would be brought to the Nahariya hospital.
The simulations were held in a shock-trauma wing of the fortified emergency department, which was opened in 2012 to withstand missile attacks. The late physician Shaul Shasha, the hospital’s director general at the time, pushed for the fortification.
We hope we’re training and training and training but won’t need to treat actual people because that would be our family. Everyone—every soldier, every civilian—is like family.
“They called Dr. Shasha a mad man,” Tsvi Sheleg, a physician and the hospital’s deputy director general, said of the fortified wing. “He was a visionary.”
Stepping into both the emergency department and an underground makeshift hospital is like entering a bank vault—two sets of vault doors, actually, each threshold about 1 1/2 feet thick. The fortified department was built because of the hospital’s vulnerability during the Second Lebanon War, in summer 2006, when Hezbollah shot 4,000 rockets at towns and communities in northern Israel. Back then, patients were brought to what was the only fortified area: the underground bunker. As a result, no one was harmed in the strikes.
Within hours of this month’s Hamas massacre, too, all patients were moved underground. The 775-bed hospital canceled all elective surgeries to free beds for trauma patients—soldiers and civilians—should war return to the north.
The basement vault, which until Oct. 7 was empty, has become the hospital writ small. It’s drab and no-frills, but functional and clean. During a reporter’s visit, some patients sat in bed speaking on their phones, while others chatted with visiting relatives, as they would in normal times. Printed paper signs delineated the departments of thoracics, oncology, obstetrics, pediatrics, internal medicine, and dialysis.
The three simulations practiced on Wednesday were adapted from cases emergency-department professionals treated in the south on Oct. 7, said Khaled Atalla, a physician who heads the department. In Nahariya, he anticipates treating patients with blunt trauma and crushed body parts from collapsed buildings that might result from Hezbollah missile attacks.
Fifty health care professionals from Hungary were due to visit the hospital this week to train in mass-casualty scenarios. Their visit was canceled.
“Now, we’re just doing it,” Atalla quipped. “We hope we’re training and training and training but won’t need to treat actual people because that would be our family. Everyone—every soldier, every civilian—is like family.”
In the past three weeks, the emergency department has actually treated fewer patients than normal, said Atalla. One reason is that fearful residents are remaining home, leading to fewer road accidents, he said.

Roni Albert
The hospital’s slower pace reflects the changed reality of Nahariya, an already quiet town of 60,000 residents. Only about half of all stores were open on the main commercial drag, HaGaaton Street, on Wednesday. Traffic has been far lighter on roads and sidewalks. Downtown has been ominously inconsistent: calm-before-the-storm-like one day, people filling outdoor tables at Aroma Café the next.
Digital signs at HaGaaton and Weizmann streets, like billboards countrywide, now feature Israeli flags and read, “Israel will be victorious” and “We are all in it together.” On some summer nights, and on the night of Yom Ha’atzmaut (Independence Day), stages dominate that intersection as bands entertain crowds packed shoulder to shoulder on the closed streets.
Employees of the Galilee Medical Center like to say that it is the country’s closest hospital to any border and take pride in its treating a diverse population of 660,000 Galileans—Jews, Christians, Muslims, and Druze—a rainbow of cultures that’s also apparent in the hospital’s staff.
In the hospital, one room was transformed into a day care center, its shelves and tables chock full of crayons, markers, puzzles, and board games. Several little girls sported face paint: an Israeli flag, a rainbow, a butterfly. In a corridor, boys kicked a ball and shot baskets at a 3-foot-tall hoop. The day before, workers nailed low rows of hooks for the children to hang their backpacks.
Dorit Itah, who heads the occupational therapy department, explained that 80 children ages 3-14 come in each day. With no patients now and with many schools closed since the war’s outbreak, she and others were reassigned so their colleagues can continue working.
“It’s not the dream of my life to be doing arts and crafts with kids,” Itah said. “It’s like a big family in crisis time. You have to help where you can and contribute.”
The children in the room were speaking Hebrew, Russian, and Arabic.
In the lobby upstairs, Bahir Sirhan, an emergency-department physician and a Muslim who lives in the Jewish-majority town of Karmiel, spoke of treating four construction workers injured the previous week in a Hezbollah missile attack on a moshav along the border. Three were his relatives; all survived. The fourth man died.
Hezbollah’s missiles don’t recognize nationality or religion, as Hamas’ knives and bullets didn’t distinguish on Oct. 7 between Jews and Muslims, native Israelis and foreign field workers.
On matters of life and death, those in Israel, as the billboard proclaimed, are all in it together.
In what normally is the hospital’s thoracic surgery department, Rona Spector sat at a conference room table. On Wednesday, the department’s corridors were dark, the nurses station was empty, no patients walked the halls, no beeping monitors sounded, no orders echoed.
Spector, a native of the Tel Aviv suburb of Givatayim, has lived for the past 14 years outside Boston and works as a thoracic surgeon at Tufts Medical Center.

Roni Albert
Upon learning of Hamas’ attack, she and several other Boston-area Israeli doctors exchanged text messages inquiring about opportunities to volunteer at hospitals in their homeland.
A week later, she flew to Israel. Spector will remain until the end of the month, forfeiting her Tufts salary. Her bosses and colleagues supported her desire to fly to Israel to lend a hand, Spector said. She led one simulation the other day and will run one next week on opening chest airways. Spector said she’s here to help and likely won’t have time to visit her parents or in-laws in the country’s center.
The hospital has only one thoracic surgeon on staff, Moshe Lapidot, who happens to know Spector from when they both did a fellowship in Boston.
Spector’s presence “is very important” both for her medical expertise and as a morale boost, Lapidot said.
During the interview, a hospital spokesman told Spector “kol hakavod” (kudos) for coming to volunteer. She demurred.
“Not ‘kol hakavod.’ It’s my duty,” she said. If the war is prolonged, as experts predict, Spector said she’ll return to Nahariya for another stint. “My heart is here, and Israel is my identity. I prefer being here. The minute you land, you feel a sense of relief. I’m where I’m supposed to be. I’m with my people.”
Become a member of Tablet Magazine
Hillel Kuttler, a writer and editor, can be reached at [email protected].