Israel, a Leader in Transplant Tourism, Finds a Formula for Increasing Domestic Donations
Faced with rabbinic resistance and social ambivalence, the government has pioneered a program that rewards a willingness to donate
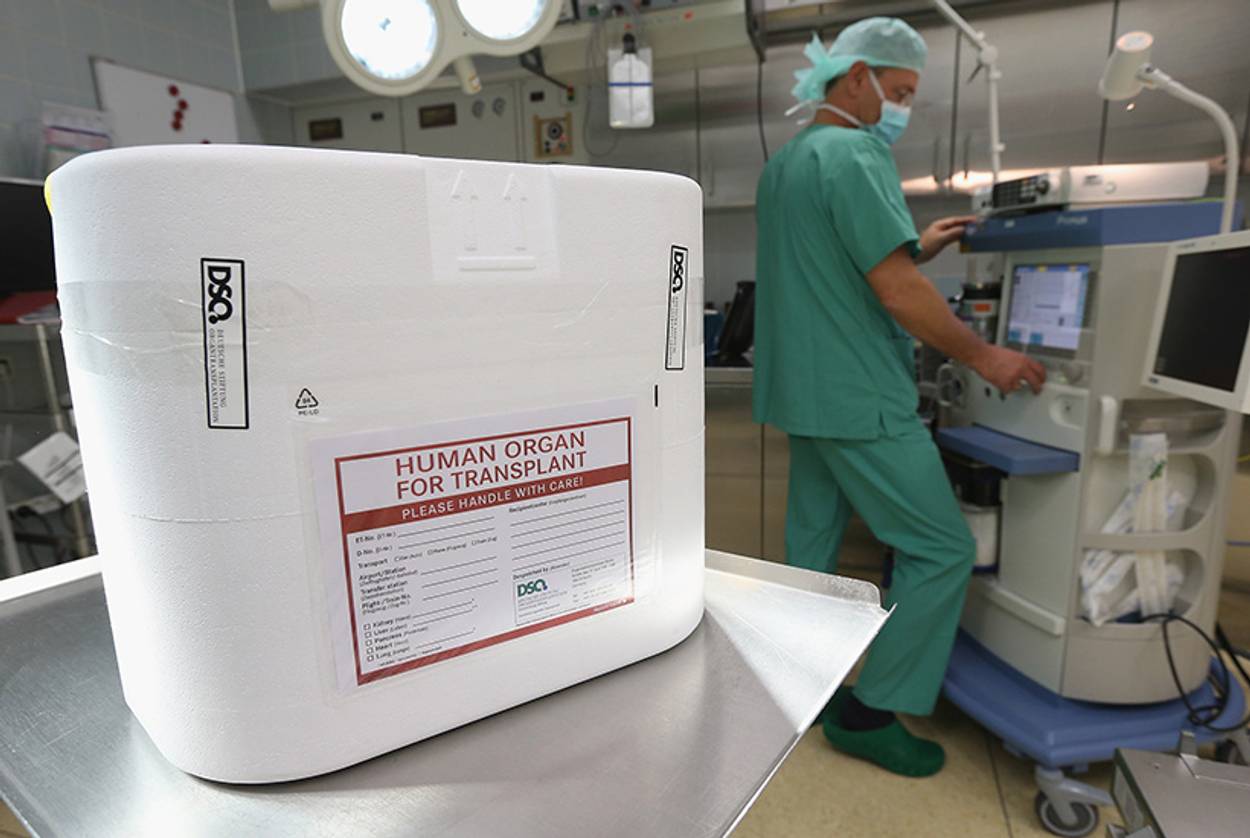



A decade ago, Israelis were among the world’s leading “transplant tourists”—a phenomenon driven in large part by Israeli insurers’ willingness to reimburse the costs of transplant operations abroad, which gave Israelis of all means access to the international organ trade. The laissez-faire stance of the Israeli government was in large part due to persistent shortages of domestic organ donors.
Yet, as horror stories about overseas organ transactions seeped into public awareness, doctors—including Jacob Lavee, director of the heart transplant unit at Sheba Medical Center in Tel Hashomer—and others began lobbying for changes to Israel’s laws governing transplants. In 2008, the Knesset ratified the Organ Transplant Act, which outlawed giving and receiving compensation for donations—both inside and outside Israel. Abolishing a commercial source of organs necessitated that Israel find a way to induce a dramatic increase in its number of donors to counterbalance the loss—immediately. Failure meant many of those waiting for transplants would die.
Increasing domestic donations is a special challenge in Israel, where religious factors have historically constrained the organ supply. Despite a 300-year-old rabbinical ruling that an autopsy—and by extension, any post-mortem surgery—can be performed to save a life, many observant Jews consider the body inviolate in death. Taboos against mutilation are less of an issue in other Western countries, where consent rates—the percentage of brain deaths that result in donation—frequently exceed 70 percent. For most of the 2000s, Israel’s hovered around 45 percent—among the lowest in the developed world.
Today, however, Israel’s consent rates have jumped, to 56 percent in 2013—still low, but a shift that demonstrates a real turnaround in public opinion surrounding organ donation. The change is largely due to the public debate surrounding brain death that followed the highly publicized decision by the family of the Israeli soccer star Avi Cohen to disregard his wishes to donate his organs after a 2010 motorcycle accident left him brain dead—and to Israel’s adoption of a unique allocation system for organs that rewards those willing to donate. At a time when waiting lists are growing everywhere, including in the United States, Israel’s success has implications for a global transplant landscape that is in dire need of innovation.
To increase public acceptance of brain death — the precondition for deceased donation — as death, Israeli legislators went to religious leaders seeking support. During traumatic events, even secular Israelis consult their rabbis. While Reform and Conservative authorities accept brain death, Orthodox rabbis are split on the issue. For some, harvesting organs from a patient with a beating heart constitutes murder. Others were willing to endorse brain death as death if the irreversible loss of brain function could be conclusively established. In 2008, to assuage the latter group and attract more advocates in the rabbinical community, the Knesset passed the Brain Respiratory-Death Act.
But the bill wound up causing more harm than good. It codified a highly restrictive testing protocol that interfered with doctors’ ability to do their jobs, and which often had to be aborted or gave results that weren’t accepted. In its first two years, it precluded enough brain-death determinations to cost Israel about 15 percent of its deceased donor pool. And it did nothing to unify the rabbinate behind brain death: Religious authorities remain split on the issue today.
However, the 2010 controversy over the death of Avi Cohen, one of Israel’s most famous soccer players, may have accomplished what the law couldn’t. After a motorcycle crash rendered Cohen, a registered organ donor, brain dead, his family publicly refused to comply with his wishes, reportedly after rabbinic authorities counseled the family against donating. The cessation of Cohen’s heartbeat shortly thereafter created a visible example of brain death as an irrevocable state. “We said in our office it was like a multimillion shekel public campaign because from that time everybody in Israel knows that brain death is death,” said Dr. Tamar Ashkenazi, director of Israel’s National Transplant Center. “It became easier to talk to families, and everybody knows now that when you talk about brain death it’s about organ donation. People go to the donor coordinator and ask them, ‘Tell me, is it like Avi Cohen?’”
But it took another two years before Israel instituted its second, and perhaps more crucial, policy response to the organ shortage—a pioneering approach that gives transplant priority to those willing to contribute to the organ pool. Launched in April 2012, the new Israeli system grants first priority for transplants to living donors and the family members of donors—who, in the event of brain death, make the ultimate decision whether to donate their kin’s organs. Registered donors of three years or more receive second priority; family members of registered donors receive a third tier of priority.
The system confers an advantage to candidates in the same tier of need; it never enables transplant candidates to supersede needier counterparts. Priority can’t catapult Status 2 recipients into the heart-transplant Status 1 list, but it can take them to the top of Status 2. With other organs, like kidneys, where a point system assigns values weighing age, waiting time, and compatibility create a 0 to 18 score, signing up as a donor can add a 1- to 5-point boost.
Priority allocation rewards a willingness to donate and penalizes free-riding behavior that in the past afforded Israelis with no intention to donate equal access to organs. This is a major departure from the status quo – Israel is the first nation to incorporate non-medical factors into organ allocation on a national scale. (It has precedents in Singapore, where opting-out of implied donor consent pushes transplant candidates down the waiting list should they need an organ, and the United States, where living kidney donors have transplant priority status should they likewise need it.)
Because registering to become a donor is non-binding, skeptics have noted that the priority system can be gamed. But Israel is the only national system that rewards the relatives of deceased donors with priority status down the road—creating an incentive, if an abstract one, for families to consent to donate the organs of their brain-dead kin in the hospital.
Orthodox Israelis opposed to organ harvesting on religious grounds have called the system discriminatory. But Lavee argues that the willingness of those same people to accept donated organs ultimately dissuaded potential donors from participating in the organ pool. “There was a dismay among the Israeli population that there were many, many free riders,” he explained. “Why should people donate if their organs would go to people who would never donate themselves?”
In 2013, the first full year of the new system, there were a record number of transplants in Israel; meanwhile, transplants received by Israeli patients abroad fell to a quarter of their 2007 peak. Most of what continues is the result of lawful allocations many nations offer foreign transplant candidates. Another feature of the 2008 Organ Transplant Act—full reimbursement to living donors for lost work time, and health and life insurance for five years—has helped spur donations of kidneys, and lobes of liver and lungs. Between 2011 and 2013, the number of Israeli living organ donors increased by 67 percent over the preceding three-year period, and the Israeli transplant waiting list contracted in 2013.
But for all it has achieved bringing transplants on par with pre-reform numbers through consensual domestic donations, Israel’s organ shortage persists. The waiting list could contract because it excludes would-be recipients over 65. Eighty-nine people, 8.2 percent of the active waiting list, died awaiting transplants that could have extended their lives. Those not content to wait idly fueled the rise of organ-trafficking rings reportedly connecting donors from a range of countries—Kosovo, Azerbaijan, Costa Rica—to Israelis willing to pay in excess of $200,000 for organs.
Nevertheless, any improvement is worthwhile. “I think there’s too much attention placed on eliminating the shortage and that if you haven’t eliminated the shortage you haven’t solved the problem,” said Alex Tabarrok, an economist at George Mason University. “Every attempted solution doesn’t have to solve the problem 100 percent.”
To that end, the United Kingdom is considering legislation that would make it the first country to adopt a “no give, no take” allocation policy. The United States, with over 78,000 people on waiting lists, needs such a reform: 18 Americans die each day waiting for organs. Taxpayers spend over $34 billion each year treating kidney failure alone, about 6.2 percent of total Medicare spending in 2011 and rising inexorably. Tacking on private insurance costs adds another $15 billion. “People realize something has got to be done,” Tabarrok told me. “Everyone knows it’s going to be worse in the future if we don’t do something.”
***
Like this article? Sign up for our Daily Digest to get Tablet Magazine’s new content in your inbox each morning.
Dimitri Linde is a freelance writer living in Cambridge, Mass.
Dimitri Linde is a freelance writer living in Cambridge, Mass.